Photo Credit: dolgachov / istockphoto.com
Overactive Bladder Treatment
A bladder that doesn’t cooperate can be more than just annoying. From independence and comfort to social life and intimacy, your overactive bladder can begin to interfere with many aspects of your life and personality, and soon you may feel like you’re at the mercy of your urge to “go”.
Of course, that’s no way to live your life, and you shouldn’t suffer any more than already have. Fortunately, there are plenty of ways to get your bladder issues under control, and if self-care doesn’t bring the improvement you were hoping for, you can team up with your doctor to craft a more aggressive OAB treatment plan with a combination of these approaches.
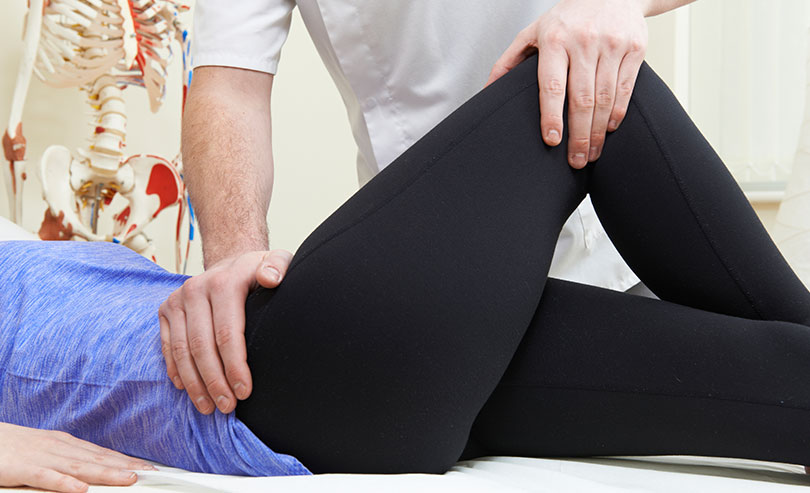
1. Bladder Training
One of the first steps to a stronger bladder is physical strengthening, and that means getting in the habit of exercising your bladder every day. You may have heard of Kegel exercises – particularly useful for women after pregnancy – but these pelvic floor contractions are more helpful for stress incontinence than they are for urge incontinence (which comes with OAB).
Training exercises for overactive bladder are more passive, but just as targeted: you will set a “pee schedule” and stick with it, and when the urge to go comes along, you force your bladder to wait. It may sound dreadfully uncomfortable, but you’ll soon find that you are able to hold it for an extra minute, then a few minutes, and eventually an hour or more.

Photo Credit: loooby / istockphoto.com
2. Diet Changes
Along with bladder training, a few strategic changes to your daily menu can have profound effects on your bladder control. There are few foods that directly improve bladder function, but plenty of ingredients are known to irritate the bladder and should be cut out of your diet. Start by eliminating diuretics like caffeine and alcohol (they both encourage the kidneys to produce more urine), and be sure to avoid irritating artificial sweeteners and acidic fruits (citrus, pineapple, and tomatoes are the worst offenders).
Water has an important role to play in your daily diet, too. It may seem like a bad idea to take in too much, but too little water will lead to constipation and concentrated urine – two conditions that are sure to irritate your bladder and increase the feeling of urgency.

Photo Credit: robynmac / istockphoto.com
3. Better Bowel Habits
The bladder and the bowel are next-door neighbors, and when one isn’t working properly, the other takes notice. Constipation is itself uncomfortable, but a full bowel will also press on the bladder, making OAB urgency and incontinence a lot worse. The constant pressure is difficult to ignore and can even lead to chronic pelvic muscle problems, which is another reason to treat constipation as quickly as you can.
Start by increasing your soluble fiber and insoluble fiber intake, since both are important for a healthy digestive tract. A selection of whole grains like barley and oatmeal, fresh and dried fruit, green veggies, and beans should get you back on track, but if diet alone doesn’t do the trick, talk to your doctor about incorporating a laxative.

Photo Credit: ebstock / istockphoto.com
4. Weight Loss
Studies suggest that losing a moderate amount of excess weight can reduce the symptoms of stress incontinence and OAB. If you can lose about 8% of your body weight – that’s around 15 to 20 pounds for many women – you will likely see remarkable results, though even just a few pounds of weight loss can reduce incontinence episodes by over 25%.
The explanation makes perfect sense: shedding pounds from the abdomen will alleviate pressure on all the organs in the area, including the bladder. And without the extra pressure, the muscles in and around the pelvic floor can once again focus on supporting the bladder.
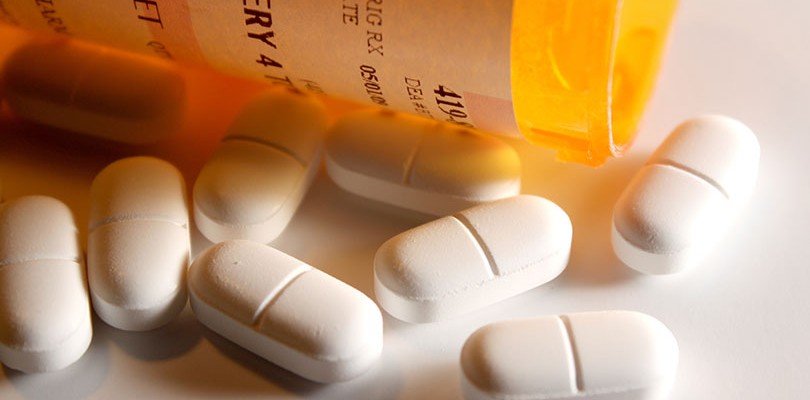
Photo Credit: dptulk / istockphoto.com
5. Anticholinergic Drugs
This specific class of medication is sometimes used to control the muscle spasms that lead to OAB. By blocking the nerve signals that typically trigger inopportune bladder contractions, an anticholinergic can reduce the frequency and severity of your urge to urinate, plus there’s some evidence that it may even increase your bladder capacity.
There are several anticholinergic drugs to choose from, though aside from Oxytrol, they all require a doctor’s prescription. Most people have very favorable reactions to anticholinergics, though there are a few possible side effects, like dry mouth, constipation, and a fast heartbeat.
Although OAB in men is chronically undertreated, it doesn’t have to hold you back. Be proactive in your health by looking out for warning signs.

Photo Credit: jes2ufoto / istockphoto.com
6. Botox
Although it’s commonly used for superficial purposes, Botox is a handy muscle relaxer for a variety of conditions, including OAB. By injecting this compound right into the bladder, many patients will experience fewer uncomfortable contractions and a better bladder capacity for up to a year after the injection.
However, Botox isn’t without its dangers: some people will find that they retain urine too much after the procedure, and that can come with pain and complications, like urinary tract infections. For these reasons, Botox for overactive bladder is only considered as a second-line of defense, and only for certain OAB sufferers.

Photo Credit: photos_ / istockphoto.com
7. Antidepressants
Certain antidepressants, like Tofranil, Tipramine, and Norfranil, can help suppress OAB symptoms, but which one your doctor chooses to prescribe will depend on your specific set of symptoms. For instance, the SSRI class of antidepressants work better for stress incontinence than for urge incontinence, although it’s not clear exactly how it helps. Alternatively, tricyclic antidepressants (Tofranil is one of the more common) are known to have anticholinergic side effects, relaxing the bladder muscle and causing the muscles at the bladder neck to contract. These work best for OAB and mixed incontinence.

Photo Credit: kamolmek / istockphoto.com
8. Natural Supplements
While there have been few scientific studies on herbal remedies as an option for overactive bladder treatment, some remedies have shown promising results for some people. For example, studies out of Japan have shown improvement in urgency, leakage, and nighttime urination with an herbal preparation known as gosha-jinki-gan, while the buchu plant from South Africa is thought to nourish the bladder tissue and fight inflammation that can lead to infections and incontinence. There are also plenty of everyday herbs that may help with symptoms, including corn silk and capsaicin (the active ingredient in chili peppers). But remember that herbs can be powerful – consult your doctor before adding any into your OAB management plan.

Photo Credit: Stuart Jenner / istockphoto.com
9. Nerve Stimulation
If lifestyle changes and medication can’t control your OAB symptoms, your doctor may recommend a slightly more invasive approach for long-term relief. A procedure known as nerve stimulation involves implanting a small electronic device in the body, a “pacemaker” that sits under your skin and sends electrical impulses to the sacral nerve, which plays an important role in bladder emptying. The aim is to strengthen the supportive muscles and lead to better bladder control, though there’s no guarantee that the procedure will eradicate all your symptoms.
Photo Credit: kzenon / istockphoto.com
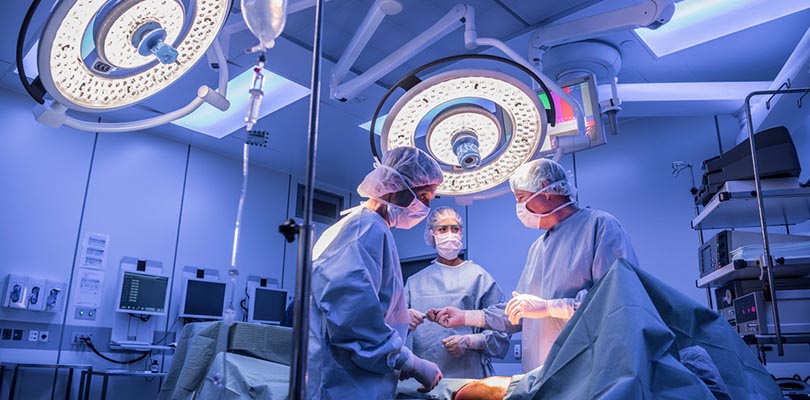
10. Bladder Augmentation Surgery
When all other approaches to strengthen and retrain the bladder have failed, you may need to alter the bladder itself. Typically used as a last resort in only the most serious cases of OAB, bladder augmentation involves enlarging the bladder with a section of your large intestine, so there’s physically more space to store urine, and therefore less pressure to urinate. This is the most invasive and complex procedure for solving OAB, and so it carries the longest recovery time and lasting consequences. Once you have bladder augmentation surgery, you will no longer be able to urinate naturally – you will have to use a catheter or stoma from now on.
The good news is that many, if not most cases of OAB can be very well controlled with a commitment to bladder training and good lifestyle changes, and the road to improvement is sometimes surprisingly short.
Read more about overactive bladder treatments over at NewLifeOutlook.
What causes overactive bladder? We go over some of the potential reasons why you may be experiencing OAB symptoms and what treatments are.